Can a Leftover Tooth Root Cause Pain After Extraction?
 In early January, I had my lower right wisdom tooth removed. The dentist wouldn’t allow me to handle or keep the tooth. My gum needed three weeks to close, which made me question whether everything was healing normally.
In early January, I had my lower right wisdom tooth removed. The dentist wouldn’t allow me to handle or keep the tooth. My gum needed three weeks to close, which made me question whether everything was healing normally.
Not long after the procedure, I developed pain on the right side of my face, in my ear, and in the back of my left eye. While the facial and ear pain has decreased a bit, the discomfort behind my eye persists. I wonder whether a piece of the tooth may still be in the socket and causing an infection. Would that explain why my dentist wouldn’t let me see the tooth? Thanks. Nida from MD
Nida,
After a wisdom tooth extraction with an open socket, infection is uncommon because fluids can drain naturally. Infections occur more often when an impacted tooth requires stitches that close the gum over the site.
If a full root or a large fragment remains in the socket, the gum can heal over it, trapping bacteria in the jaw. This situation may lead to persistent pain, swelling, or infection.
Why Might Symptoms Linger After Tooth Extraction?
Lingering symptoms may require evaluation from another dentist, ideally an oral surgeon who can both diagnose and treat the problem. An X-ray provides the clearest way to see whether any tooth structure remains.
This process helps determine:
- Whether a retained root is causing symptoms
- Whether the bone has already healed over the area
- How complex the removal would be if needed
If a significant root was left behind, requesting a refund could be a reasonable next step.
Why Might a Tooth Root Fracture During Extraction?
Tooth roots sometimes break during removal, particularly in older adults whose roots may thicken over time. This complication can happen even with careful treatment and does not necessarily reflect poor care.
Appropriate management depends on the fragment size:
- Small tips in sensitive areas may remain without causing harm
- Larger pieces typically require removal by the dentist or an oral surgeon
Patients should always receive a clear explanation when this occurs.
Many patients want to see or keep their extracted teeth, and dentists often honor that request. If you asked but could not view the tooth, seeking clarification or another opinion would be reasonable.
Dr. Thaddeus Michalski, a Rocky Hill, Connecticut dentist, sponsors this post. Read why many of his patients say he is one of the best dentists in town.
Will I Regret Not Getting a Tooth Extraction and Dental Implant?
I had a root canal in 2020 without any problems until now. The tooth has hurt on and off for the past month, but now it’s starting to throb. I am afraid that I will need an extraction. Is it worth repeating a root canal, or would I regret not getting an extraction and a dental implant? – Thanks. Elias
Elias
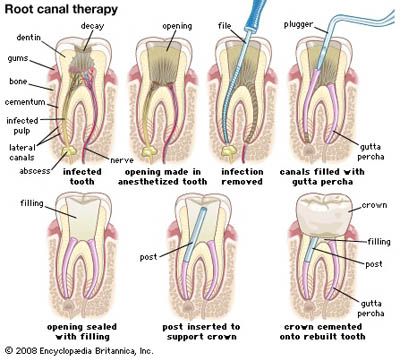
Root canal failure can be frustrating and painful. It happens when a tooth doesn’t heal completely after a root canal treatment, leading to recurring symptoms. Your symptoms may be the result of root canal failure.
What Causes Root Canal Failure?
A hidden tooth infection or curvy tooth roots can contribute to root canal failure:
- Hidden infection: It can be challenging for a dentist to remove all the infection from a tooth’s complex root canals. Even a tiny amount of remaining bacteria can cause problems later.
- Curved or branching roots: These can make it hard to reach and clean all areas of the tooth.
What Are the Treatment Options for Root Canal Failure?
The treatment options for root canal failure are retreatment, root canal surgery, or extraction and a dental implant for an unsavable tooth.
- Retreatment: A dentist can attempt to clean the infected area and seal it again.
- Root canal surgery: A dentist or specialist must access the tip of a tooth near the gumline and through the bone to remove the infection. An endodontist (root canal specialist) typically performs this procedure (apicoectomy).
- Extraction for tooth fracture or an unsavable tooth: A crack in the tooth can also lead to pain and infection. Unfortunately, saving a tooth with a severe fracture can be challenging.
See a dentist with extensive root canal treatment experience or an endodontist to discuss your options.
Dr. Thaddeus Michalski, a Rocky Hill, Connecticut dentist sponsors this post.
Why Do I Have Pain Weeks After a Tooth Extraction?
Last month, my dentist sectioned my upper right molar into three pieces before extracting it. It was a fractured root canal tooth that the dentist couldn’t save. Since the extraction, I’ve had late afternoon and evening pain that ibuprofen doesn’t relieve. I feel pain on the side of my face, too. It throbs into my ear. My dentist said that if it persists, she can prescribe an antibiotic. Shouldn’t she try to figure out the cause instead of just prescribing meds? Thanks. Avery from NV
Avery,
It’s normal to experience discomfort after a tooth extraction for about a week. However, if the pain persists and worsens, especially for weeks, see a dentist.
What Causes Persistent Pain After Tooth Extraction?
A latent infection in the extraction site is one potential cause of persistent pain after a tooth extraction. An infection may require antibiotic treatment.
Another potential cause could be pain from an adjacent tooth or a nerve. In your case, the numbness you’re experiencing might indicate pressure on a nerve.
Schedule an Exam and X-ray
We recommend scheduling a follow-up appointment with your dentist to assess the situation. She can examine and x-ray the area, rule out any potential complications, and recommend appropriate treatment.
If your dentist determines you have an infection, an antibiotic like clindamycin may help. Take all the medication as prescribed to prevent a recurring infection. If you are considering tooth replacement and want a dental implant, notify your dentist so that she can create a treatment plan for an implant.
Dr. Thaddeus Michalski, a Rocky Hill, Connecticut dentist and Diplomate of the International Congress of Oral Implantologists, sponsors this post. Read how he strives to provide some of the best dental care in Rocky Hill.
Do I Need a Tooth Root Removed That Broke During Extraction?
When my dentist removed my upper left first molar, part of the tooth root broke off. My dentist referred me to an oral surgeon to remove the root. Is there any harm in leaving the root in the socket? How common is this, anyway? I’m a little frustrated that my dentist could have referred me to a surgeon in the first place. He wounded so confident about the extraction that I trusted him. Thanks. Leander from S. Dakota
Leander,
Part of a tooth root may break during tooth removal because of the root shape or challenges removing the tooth; it is not uncommon. If a dentist realizes a root fragment is left, they may refer you to a specialist. Other dentists use an X-ray to anticipate the complexities of extraction and may refer you to a specialist upfront for tooth removal.
Do You Need to Remove a First Molar Tooth Root?

If a dentist leaves a tooth root behind after extracting an upper first molar tooth, the root can poke the sinus, resulting in sinus perforation. Leaving the tooth root in the socket for months increases complications and risks. Sinus perforation surgery can be complex and requires the skill of a specialist.
We recommend getting a second opinion right away. If the tooth root is too close to the sinus wall, a specialist may decide to leave it. Otherwise, the surgeon will remove it promptly.
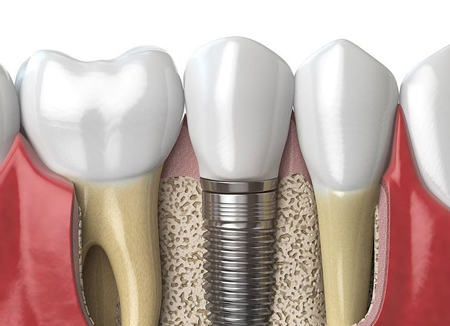
If you are considering a dental implant to replace the missing first molar tooth, talk to the surgeon about it. Depending on the condition of the tooth socket and your sinus, the surgeon may recommend a bone graft or sinus augmentation procedure to prepare the site for an implant. A dental implant needs enough quality bone to support an implant crown. Caring for the socket now can prevent the need for another surgery later if appropriate. Ask the specialist about your options.
Dr. Thaddeus Michalski, a Rocky Hill, Connecticut dentist and Diplomate of the International Congress of Oral Implantologist, sponsors this post.


